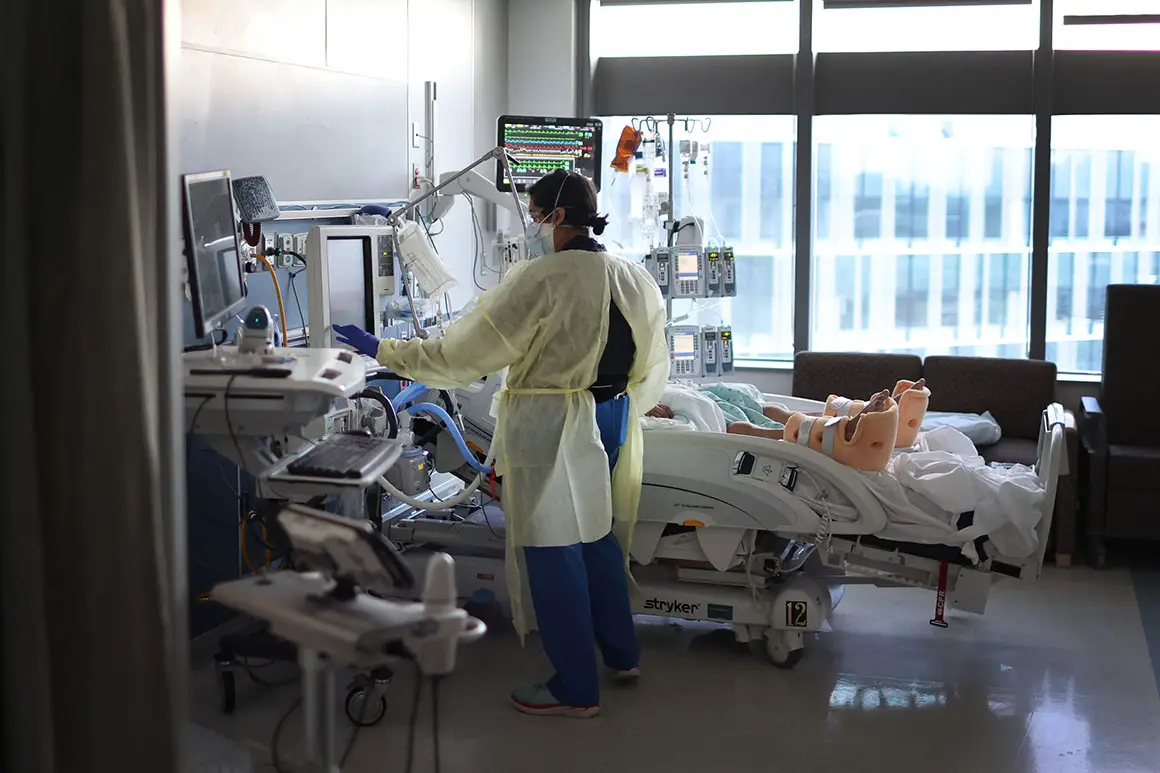
A record 4,734 patients were recorded as having caught Covid-19 in-house on Jan. 19.
During the January Covid-19 surge a year ago, hospitals reported around 2,000 patients each week on average had contracted Covid during their stay, compared to roughly 3,000 this year.
The total number of people who contract Covid-19 while in the hospital remains unclear because these figures only count patients who were in the hospital at least 14 consecutive days and don’t account for people who test positive after leaving. The government’s figures are likely a fraction of the total.
Hospital-acquired infections have long been one of the most serious risks for patients, especially those who stay for weeks or months. But the recent data show that more than two years into the pandemic, hospitals still have a long way to go to prevent transmission within their walls.
Michael Osterholm, an epidemiologist at the University of Minnesota, said he’s concerned about the rise in infections. “Using standard infection control, that shouldn’t happen where there is transmission occurring, whether it be between patient to patient, visitor to patient or worker to patient,” he said.
He said hospitals aren’t doing enough to prevent transmission, allowing visitors and staff to wear surgical masks rather than more protective N-95 masks. The Centers for Disease Control and Prevention hasn’t recommended that all health care workers and visitors wear N-95s at all times.
Despite the Omicron-related spike, US health officials haven’t decided whether to suggest hospitals revamp their infection control measures, three officials told POLITICO. The figures are preliminary, and CDC officials are investigating what caused the increase, said two of the officials, who were granted anonymity because they weren’t authorized to speak publicly about internal discussions.
One potential factor, several public health experts said, is the CDC’s decision in December to allow health workers who had tested positive for Covid to return without first isolating or testing to ensure they were no longer infectious. However, several public health experts also said that decision likely had minimal impact because workers wear masks and ideally higher grade N-95s.
A CDC spokesperson declined to comment on whether the agency’s decision played a role.
It isn’t known what other factors, if any, might have influenced the increase, though some public health experts aren’t surprised.
“A hospital is a subset of the population,” said Kathleen Gallagher, an epidemiologist at the National Patient Advocate Foundation. “You’d expect to see that increase.”
“At the time, home tests were scarce, lines were hours long for in-office testing, and other changes were going on, like CDC changes to healthcare worker quarantine procedures,” she added. “People visiting patients were potentially not required to show proof of vaccination, and may not have worn the right masks or worn them improperly.”
The number of patients who catch Covid at hospitals tracks community infection rates nationwide, POLITICO’s analysis of the data shows. Last summer, for instance, when cases across the country were much lower, so were cases of hospital transmission.
Despite the January spike, the chance of catching Covid-19 at a hospital is relatively low, federal and state health officials said.
For example, in North Carolina, 1.6 percent of patients got infected with Covid-19 at a hospital in December of last year, according to a state health department spokesperson. That percentage rose to 2.2 percent in January. On average, 25 patients each day acquired infections at the hospital in December, compared to 96 in January, on average, the spokesperson said.
Shama Cash-Goldwasser, senior technical adviser at Resolve to Save Lives, a group run by former CDC director Tom Frieden that aims to prevent epidemics, said it’s impossible for hospitals to bring transmission to zero, particularly when facilities are crowded and staff are overwhelmed as they have been during Covid-19 surges. “It’s unfortunate,” she said. “I’m not saying it’s OK … Immunocompromised patients and very sick people are at very high risk of poor outcomes, so transmission inside a hospital can really be devastating.”
The figures don’t say which hospitals accounted for the most transmission. The Department of Health and Human Services, which compiles the data, doesn’t release per-hospital numbers. The figures are compiled as part of a daily survey of hospitals reporting how the pandemic affects their operations, from case loads to equipment supplies.
US health officials are considering changing how hospitals report the number of patients who contract Covid-19 in-house, POLITICO has reporteda change that could set off concerns from hospital lobbyists and associations that say such transmission is rare.
But the change would make it easier to spot how many patients in a given day are suspected to have contracted Covid-19 at hospitals, POLITICO reported. The discussions, which have involved officials from the CDC and HHS, might not result in any changes.